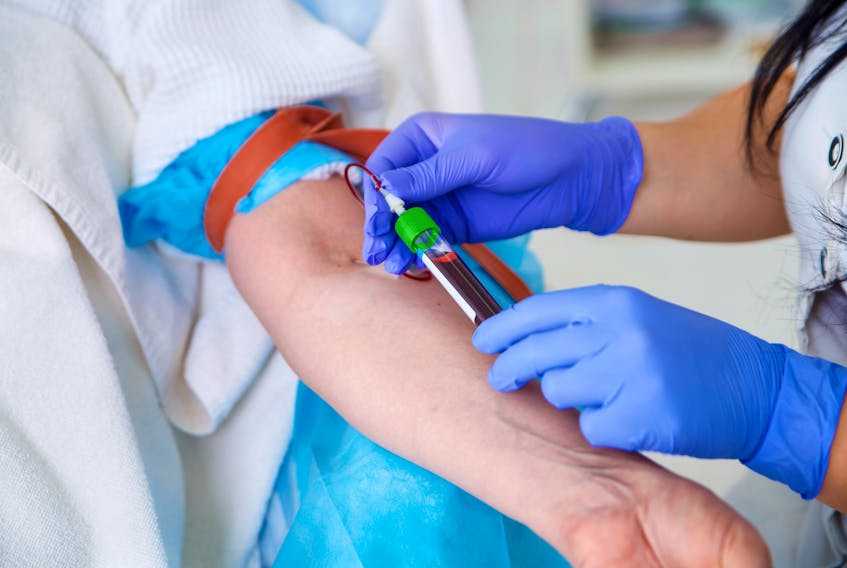
For many years, people usually did their routine blood tests on an empty stomach. Inevitably, this caused a major congestion in the hospital every morning as people lined up at the blood testing centre in a queue that would spiral around corners and down hallways as people waited, sometimes for hours, to get tested.
Getting your routine blood tests on an empty stomach was important mainly because of the tests to check blood sugar and cholesterol. Most other blood tests, like hemoglobin levels, renal function, liver function, thyroid hormones, sodium and potassium levels don’t need to be done on an empty stomach because they do not change before or after meals to any meaningful degree.
Blood sugar, of course, does change with meals and will often spike after you eat something, especially something very sugary or starchy. So, for many years, physicians used fasting blood sugar levels to test for and follow-up on diabetes. There are a few problems with testing blood sugar levels, and over the past few years this has largely been replaced by testing Hemoglobin A1c (HbA1c). HbA1c gives you a three-month average of your blood sugar control and is therefore immune from the fluctuations that we often see with single blood sugar measurements. These don’t need to be done an empty stomach.
This left only cholesterol. Cholesterol, too, can be affected by eating in the hours before a blood test. This occurs because the type of cholesterol people are usually most interested in, the LDL or bad cholesterol, is not actually measured in your blood but calculated using a mathematical formula. By measuring the total cholesterol, the HDL or good cholesterol and another type of cholesterol called triglycerides, the computer doing the analysis can automatically generated a level for your LDL that is often very accurate. LDL can be measured directly in the blood, and sometimes this is done in research protocols, but for practical reasons and reasons of economy, calculated LDL values were usually quite sufficient.
Still though, because triglycerides can rise sharply after a meal and because high triglyceride levels can throw off the LDL calculations, getting your cholesterol checked on an empty stomach was generally recommended.
However, the thinking on this matter has evolved recently. Over the past few years, research has shown that cholesterol levels change very little after normal meals. One study in Circulation found that after meals the maximum change in LDL was only 0.2 mmol/L, which is too small a change to be clinically meaningful.
Recently, another study in JAMA Internal Medicine tested fasting vs. non-fasting cholesterol levels. This study agreed with the prior research that there was little difference in cholesterol levels. When it came to classifying people as high vs. low risk, in other words in deciding whether they needed to start medication, they also found excellent agreement between fasting and non-fasting blood tests as the cholesterol tests were in agreement 94.8 per cent of the time.
There may be specific situations where early morning blood tests are required. Certain hormones, like testosterone or cortisol, need to be measured in the early morning in order to be interpreted properly because they fluctuate quite a bit during the day. However, they need to be done early in the morning, not necessarily on an empty stomach.
For the routine blood tests that most people get on an annual or semi-annual basis, there seems to be little reason to ask for fasting blood tests and both the Canadian and U.S. cholesterol guidelines seem to be endorsing this view. While there may be specific situations where an early morning fasting blood test is necessary, most people can probably eat breakfast first. They can also probably sleep in, too.
Christopher Labos is a Montreal doctor and an associate with the McGill Office for Science and Society. He also co-hosts a podcast called The Body of Evidence.
Copyright Postmedia Network Inc., 2019