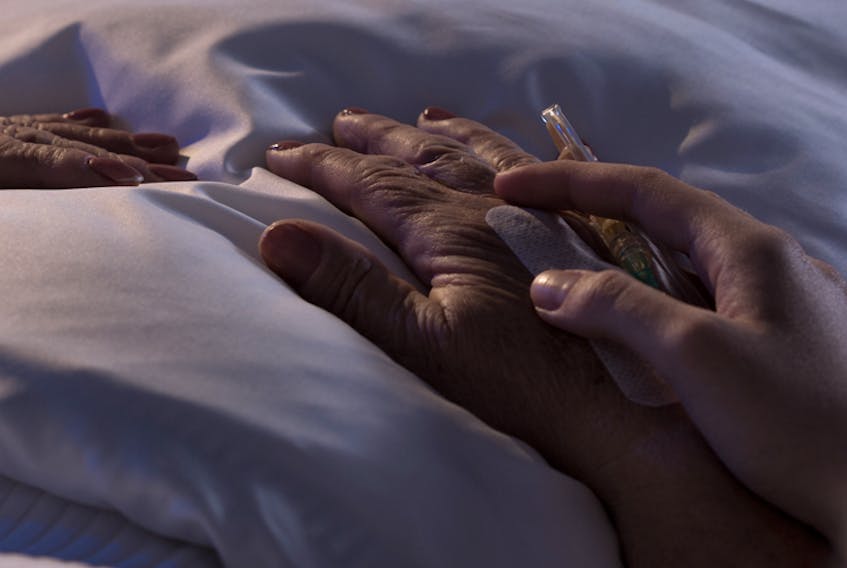
Thirteen years after Nova Scotia's first purpose-built palliative care unit opened in the Aberdeen Hospital in New Glasgow, the challenges are new and growing but the spirit to meet them remains strong.
Dr. Anne Kwasnik left 30 years of family practice to become its medical director two years ago.
“It is extremely gratifying when we can ease the stress and strain on the patient and the patient’s family. We can do that through a wide range of aids and comforts as well as pain medication,” she said.
It's that ability to alleviate suffering and restore dignity that lured the mostly-retired Dr. Gerry Farrell away from his family medicine practice to work exclusively in the largely uncharted field of palliative care.
“We’re very fortunate in Pictou County to have a long-established program, the support of the Aberdeen Palliative Care Society and a community that generously donates time and money," he says.
"There are areas in Nova Scotia that still don’t have access to palliative care, which is not surprising when you consider only 30 per cent of Canadians have access."
While programs vary from place to place, the Aberdeen’s program began in the community and the six-bed hospital unit, resembling a high-end hotel, opened in 2006. The program aims to help patients and families understand a diagnosis and assess treatment options. It also provides social, psychological, emotional and spiritual support to the patient, family, and friends. Recently, music therapy and bereavement counselling have been added.
Case by case

Kwasnik said taking the time to get to know each person and their goals is vital to the program.
“If all our staff is dealing with an elderly person with co-morbidities who has had a good, long life, the conversations may be very different from when it is a young person with an aggressive disease," she explains.
"In the latter case, death is coming much sooner than expected and that person often feels a need to form some sort of legacy for themselves, for their loved ones.”
She acknowledged most people hope to die at home, adding it is often possible with supports in place.
“But for some, a time comes when home is not the best place to be and there is better care in the hospital. Often, by that time, everyone is OK with that.”
Kwasnik, who left Chicago with her physician husband and their three children in 2003 for a more rural life in Nova Scotia, is quick to point out the demands on the program are growing.
“In our rural area, we have a rapidly aging population. We don’t have families encapsulated in one geographic area to the extent we once did so practical, physical supports may not be there for a patient.”
She would like to see all health care professionals get some training in palliative care.
“In many cases, the palliative process could start with the family physician rather than passing the patient off to the program, but I’m well aware of the current demands on those physicians.”
Farrell, the program’s first medical director, delayed his retirement to give Kwasnick time to do a residency in palliative care because he thought she was right for the job. His own interest in the field was ignited when, having just delivered a baby in the early-morning hours, he was asked to look in on a woman who was dying.
“She was suffering greatly. I’d been with dying patients before but it struck me there was so much to learn and such a need to learn," he says.
Always learning
Kwasnik joked that she was older than the instructors, let alone the other residents, when she trained in palliative care. But, when Farrell was getting into the field, a palliative care residency did not exist. He had to organize his own training by studying the work of British palliative care pioneer Dr. Cicely Saunders and engaging with a physician in Toronto.
“As physicians, we instinctively want to do all we can to save a patient, but in the case of palliative care, it is about finding the right thing to do rather than how many things we can do. It is also the least expensive care to provide because it does not depend on a lot of expensive, high-tech modalities which are required in other aspects of medicine.”
During her residency, Kwasnik researched the value of music in palliative care. Since then, she has convinced four organizations to share the cost of a music therapist.
“For many patients, music can be a great comfort, a joy even," she explains. "We’ve seen it reduce stress and agitation, which can decrease the need for medication. It is a relatively low-cost therapy with no side effects.”
Wendy Caldwell, who is a caregiver to her 82-year-old mother, who suffers from dementia and other health issues, witnessed the benefits of music therapy while her mother was in the Aberdeen’s palliative unit.
“There is nothing that helped my mother as much as being introduced to music therapy," Caldwell says. "She calms right down and the next thing she is singing along, asking for other songs.”
Now that her mother is out of the hospital and being cared for at home, music is improving her quality of life.
“If she is agitated or tense, we know Patsy Cline or Englebert Humperdinck can settle her better than any pills in a bottle. As a daughter who loves her mother dearly, I just can’t tell you how much it means to see her have comfort and happiness at this stage.”
"As physicians, we instinctively want to do all we can to save a patient, but in the case of palliative care, it is about finding the right thing to do rather than how many things we can do."
- Dr. Anne Kwasnik
Growing demands
Like Kwasnik, Farrell also worries about growing demands on the program.
“Early on, palliative care was mostly available to those diagnosed with cancer, but only 25-30 per cent of us will die of cancer. People are living longer with illnesses and a large number of those now receiving palliative care suffer from end-stage heart disease, end-stage renal disease, and end-stage lung disease, as well as multiple sclerosis, amyotrophic lateral sclerosis and other life-limiting diseases,” he said.
Given that people are living longer with disease, it might be expected that death and dying have been openly discussed, but Kwasnik has learned not to count on it. And people change their minds.
“Even in my own family, I was surprised by some of my mother’s wishes. It helps if we can talk openly and often about dying and death. It can make things a little easier.”
The power of palliative care support

Ian Bos first turned to the Aberdeen Hospital’s palliative care program in desperation. He’s since become a hardworking ambassador.
In the fall of 2015, he left his job in Victoria, BC, to return home to Bridgeville to help his mother and sister care for his father Ted, who had been diagnosed with terminal lung cancer a few months before.
“My dad wanted to stay at home and they were struggling to care for him as his disease progressed. His care was taking quite a toll on my mother,” Ian said.
After one particularly bad night during which Ted Bos struggled to breathe, Ian contacted a friend who had a family member in palliative care.
“I was strongly encouraged to call directly and ask for help,” he said.
One day after his call, nurse Rhonda Langille and then-palliative care director Dr. Gerry Farrell arrived at the Bos home.
“Within minutes of meeting Rhonda and Gerry, we saw some of the strain on my dad lift. The rest of the family realized we were no longer alone on this journey and that was a tremendous relief.”
With management from the palliative care team, Ted’s quality of life improved significantly. He died at home, according to his wishes, but not before Ian told him he was going to walk across Canada to raise awareness of and funds for palliative care. It took more than five months and raised $26,000. Throughout his trek, he connected with individuals and families who had used or yearned for palliative care services.
“I connected with amazing people, many of whom I am still in contact with. I learned about existing palliative services, and very often, about the limitations and lack of services.”
At the end of the walk, Bos returned home to come to terms with his father’s absence.
“I decided if I could find work — and I did — I’d stay in the area and I’d see if there were other ways I could help to raise awareness and improve palliative care services which I have come to see as vital.”
As a board member of the Aberdeen Palliative Care Society, he has been involved in a series of community partnerships that lessen the load on families in palliative care. These include making available free passes to the Museum of Industry, the Pictou County Y and the Pictou County Wellness Centre. Another partnership with CHAD, an accessible transit service, helps provide transportation to medical appointments and yet another business, Our Turn to Cook, offers healthy meals to those in the program.
Margaret Ellen Disney, a trained palliative care volunteer who chairs the support society, knows people worry about dying in pain and about being a burden to their families, either financially or in terms of time.
“A terminal diagnosis can be very isolating. There is so much fear, so much worry and so much palliative care can do to help.”
Three-quarters of the society’s board are volunteers while the remaining quarter is palliative care staff.
“We work hand in hand. They advise us of their needs and we try to supply them. We try to fill the gaps by providing such things as wheelchairs, home oxygen beds and medications that are not covered.”
Disney believes families and friends should find the time to discuss death and dying.
“The outcome is the same for all of us but many of us can’t talk about it. By raising awareness, we hope we are on the road to change. It is a shame to only learn of palliative care when you need it.”
RELATED:
- Project at Yarmouth hospital will enhance support for patients and families during end-of-life care
- JILL ELLSWORTH: Providing comfort, care and hope - Hospice societies changing the lives of Nova Scotians
- Made in Canada solutions: answers to seniors' care challenges can start at home
- ALLY GARBER: The first fond farewell at Hospice Halifax